
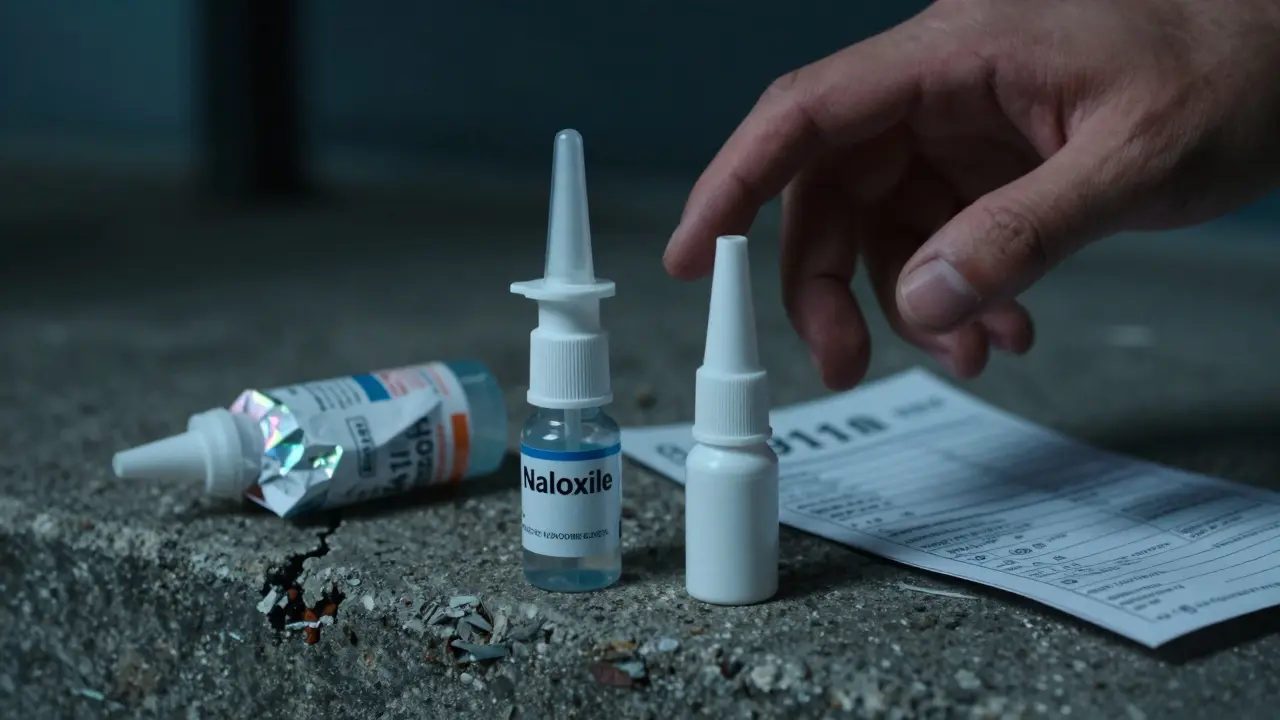
When someone overdoses on opioids, every second counts. Breathing slows down-or stops. Skin turns blue. They can’t wake up. This isn’t a movie scene. It’s happening right now, in homes, parks, and alleyways across the country. And the difference between life and death can come down to one small device: a naloxone nasal spray.
Since March 2023, naloxone nasal spray has been available over the counter in the U.S. You don’t need a prescription. You can buy it at pharmacies, community centers, or even online. It’s not a cure. It’s a pause button. A chance. And knowing how to use it could save someone’s life-maybe even someone you love.
What Naloxone Does (And What It Doesn’t)
Naloxone works by kicking opioids off the brain’s receptors. When someone overdoses, opioids like fentanyl, heroin, or oxycodone lock onto these receptors and shut down breathing. Naloxone pushes them out. It doesn’t hurt. It doesn’t get you high. It doesn’t work on alcohol, benzodiazepines, or cocaine. But if opioids are the problem, naloxone can bring someone back to life in minutes.
The standard dose in NARCAN Nasal Spray is 4 mg-enough for most cases. But with powerful synthetics like fentanyl, one dose often isn’t enough. Studies show over 30% of fentanyl overdoses need two or more doses. That’s why having more than one spray on hand matters.
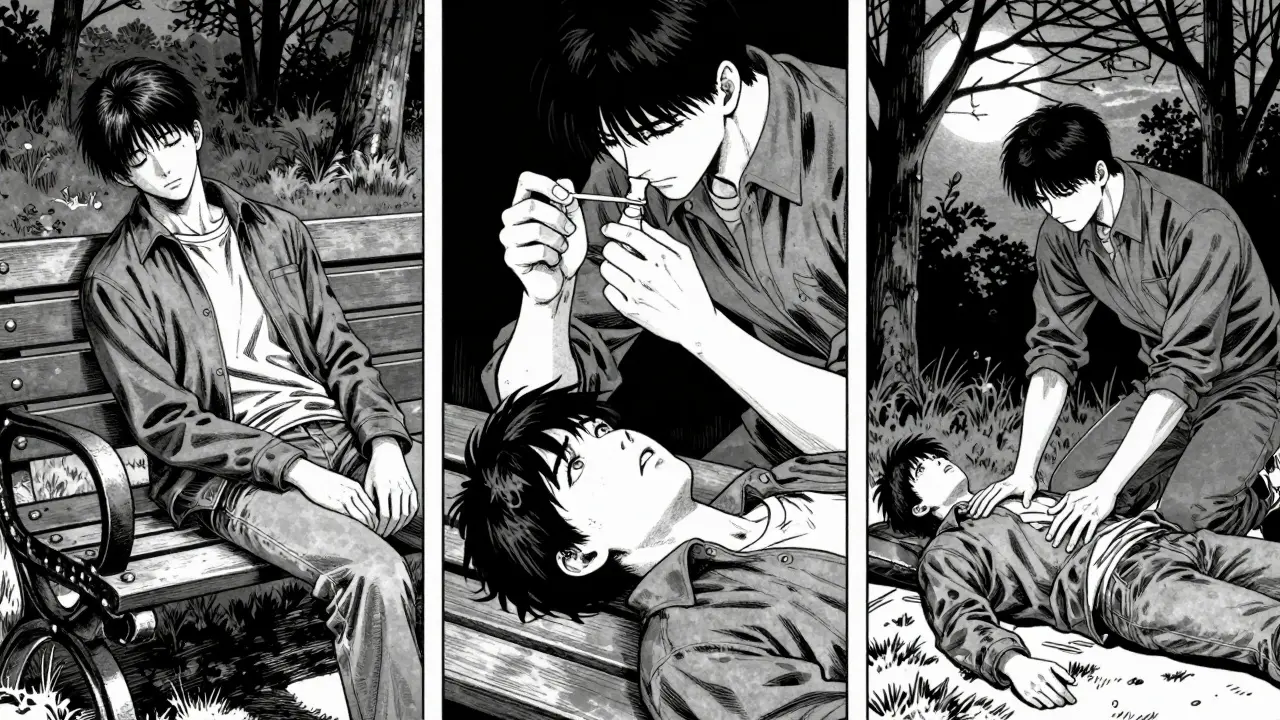
Step-by-Step: How to Use Naloxone Nasal Spray
There’s no time for panic. There’s no time for hesitation. Here’s what to do-clear, simple, and in order.
- Call 911 immediately. Don’t wait. Don’t think they’ll wake up on their own. Call before you even touch the spray. Emergency responders need to know what’s happening. Even if naloxone works, the person still needs medical care.
- Check for signs of overdose. Are they breathing? Less than 12 breaths per minute? Or not at all? Are their pupils tiny, like pinpricks? Do they slump over and won’t respond when you shake them or rub their sternum hard with your knuckles? Is their skin pale or bluish? If yes, they’re likely overdosing.
- Position them on their back. Gently lay them flat. Tilt their head back slightly to open the airway. This helps them breathe easier once naloxone kicks in.
- Remove the spray from the package. Don’t press the plunger yet. The device is pre-filled and ready to go. No assembly. No needles. Just peel the plastic backing and pull the cap off the nozzle.
- Insert the nozzle into one nostril. Gently slide it in until your fingers touch the bottom of their nose. About half to one inch deep. Don’t jam it. Just insert it snugly.
- Press the plunger firmly. Push down hard and steady until the entire dose is delivered. You’ll hear a click. Don’t stop until the plunger is fully depressed. If you don’t press all the way, you won’t give the full dose-and that could cost them their life.
- Remove the spray. Once the dose is given, pull the device out. Don’t reuse it. It’s single-use. Put it aside.
- Wait 2-3 minutes. Watch their chest. Are they breathing now? Are they stirring? If they start breathing normally-12 to 20 breaths per minute-they may be coming around. But don’t assume it’s over.
- If no response, give a second dose. Use a new spray. Put it in the other nostril. Press the plunger again. Many overdoses, especially from fentanyl, need two doses. Don’t wait. Don’t hesitate. Give it.
- Put them in the recovery position. If they start breathing but are still unconscious, roll them gently onto their side. Bend the top knee for stability. This keeps their airway open and prevents choking if they vomit.
- Stay with them for at least 4 hours. Naloxone wears off in 30 to 90 minutes. Opioids? They can stick around longer. Fentanyl, carfentanil, or other synthetics can re-overdose someone once the naloxone fades. Keep monitoring. Watch for signs they’re slipping back. If they stop breathing again, give another dose if you have it.
What to Expect After Administering Naloxone
Some people wake up confused. Angry. In pain. That’s normal. Naloxone doesn’t just reverse the overdose-it also triggers sudden opioid withdrawal. Symptoms can include nausea, vomiting, sweating, shaking, or even aggression. It’s not the drug’s fault. It’s the body reacting. Stay calm. Reassure them. They’re alive. That’s what matters.
Don’t let them leave. Don’t let them take more drugs. Even if they say they’re fine, they’re not. The risk of a second overdose is high. Emergency services need to evaluate them. And if they refuse help, stay with them until help arrives.
Common Mistakes and How to Avoid Them
People make mistakes-even in emergencies. Here are the most common ones, and how to avoid them.
- Not calling 911 first. Some people think naloxone is enough. It’s not. Medical help is still needed.
- Not pressing the plunger all the way. A 2022 study found 18% of first-time users didn’t fully depress the plunger. Practice with a training device. Or just remember: press hard until it clicks.
- Using only one spray. If they don’t wake up in 2-3 minutes, give a second dose. No shame. No delay.
- Leaving them alone. Even if they wake up, they can crash again. Monitor for at least 4 hours.
- Not recognizing overdose signs. Not everyone passes out. Some just stop breathing. Others look like they’re sleeping too deeply. Learn the signs. Carry a pocket card.
Where to Get Naloxone Nasal Spray
You can buy NARCAN Nasal Spray without a prescription at most pharmacies-CVS, Walgreens, Rite Aid, and independent drugstores. The price varies. Some packs cost around $45 with insurance. Without insurance? Around $140 for a two-pack. But many community groups, harm reduction centers, and public health departments give it out for free. Search online for "free naloxone near me"-you’ll find local programs.
Some states also have mail-order programs. In Manchester, local health clinics and needle exchanges often carry naloxone kits. Ask. They won’t judge.
Why This Matters More Than Ever
In 2022, over 81,000 Americans died from opioid overdoses. Fentanyl was involved in nearly 90% of those deaths. It’s stronger than heroin. It’s cheap. It’s mixed into pills, powders, even fake Xanax. You can’t tell by looking.
But here’s the good news: naloxone works. In communities where it’s widely available, overdose deaths drop by up to 14%. One study found that 89% of people who used naloxone nasal spray successfully reversed an overdose. That’s not luck. That’s science.
And it’s not just for drug users. It’s for parents, teachers, coworkers, friends. It’s for anyone who might be there when someone needs help.
Training Is Easy. Practice Makes a Difference.
You don’t need to be a nurse. You don’t need to be a doctor. You just need to know what to do. The CDC found that 92% of people learn how to use naloxone correctly after just 15 minutes of training. Many free online videos show you how. Watch one. Then practice with a trainer device-some pharmacies give them out for free.
Keep a spray in your car. In your bag. In your home. With your kids’ school? Ask if they have a plan. Most schools now stock naloxone. You can help make sure yours does too.
Final Thought: Be the One Who Acts
Most people freeze when they see an overdose. They think, "I’m not trained." "I don’t know what to do." "What if I mess up?"
Here’s the truth: you don’t have to be perfect. You just have to act. Even if you’re scared. Even if you’re unsure. Even if you’ve never held a spray before.
Calling 911. Giving the spray. Staying with them. That’s enough. That’s everything.
One spray. One moment. One life.
Can naloxone nasal spray be used on anyone, even if I’m not sure they took opioids?
Yes. Naloxone is safe to use even if you’re not 100% sure opioids are involved. It has no effect on people who haven’t taken opioids. If they’re unresponsive, not breathing, and you suspect an overdose, give it. It won’t hurt them-it could save them.
How long does naloxone last, and why might someone overdose again after it wears off?
Naloxone works for 30 to 90 minutes. But drugs like fentanyl, carfentanil, or heroin can stay in the body much longer. Once naloxone wears off, the opioid can re-bind to brain receptors and stop breathing again. That’s why you must monitor the person for at least 4 hours and be ready to give more doses if needed.
Can I use naloxone on a child or teenager?
Yes. Naloxone is safe for all ages, including children and teens. The dose is the same regardless of weight or age. If a child is unresponsive and showing signs of overdose, administer the spray as you would for an adult. Always call 911 afterward.
Does naloxone work on fentanyl?
Yes, but it often requires more than one dose. Fentanyl is 50 to 100 times stronger than heroin. In about one-third of fentanyl overdoses, a single 4 mg dose of naloxone isn’t enough. You may need two, three, or even more doses. Keep giving it until help arrives.
What if I give naloxone and nothing happens?
If there’s no response after two doses and you’ve waited 3-5 minutes between doses, the person may have overdosed on something other than opioids-like a sedative or alcohol. But don’t stop. Keep doing rescue breathing. Keep trying to wake them. Call 911 again. They still need emergency care. Naloxone isn’t magic-it’s a tool. And rescue breathing can keep oxygen flowing until help arrives.
Is it legal to give naloxone to someone else?
Yes. All 50 U.S. states and the District of Columbia have Good Samaritan laws that protect people who give naloxone in good faith. You can’t be sued or arrested for helping. In fact, many states actively encourage bystanders to carry and use it.
Can I reuse a naloxone nasal spray?
No. Each nasal spray is single-use. Once the plunger is pressed, the device is empty and should be discarded. Never try to refill or reuse it. Always keep at least two sprays on hand.
Where should I store naloxone nasal spray?
Store it at room temperature-between 68°F and 77°F (20°C-25°C). Avoid extreme heat or cold. Don’t leave it in a hot car or freezing glovebox. It’s stable for 2 years. Check the expiration date before using.
Do I need training to use naloxone nasal spray?
No, but it helps. The device is designed for anyone to use. Most people can use it correctly after watching a 2-minute video. But practicing with a training device increases success rates from 87% to 98%. Free training is available at community centers, pharmacies, and online.
What should I do after giving naloxone?
Stay with the person. Keep monitoring their breathing. If they wake up, talk to them calmly. Don’t let them leave or take more drugs. Keep giving doses if they stop breathing again. Wait for EMS. Even if they seem fine, they need medical evaluation. Overdose can come back.






13 Comments