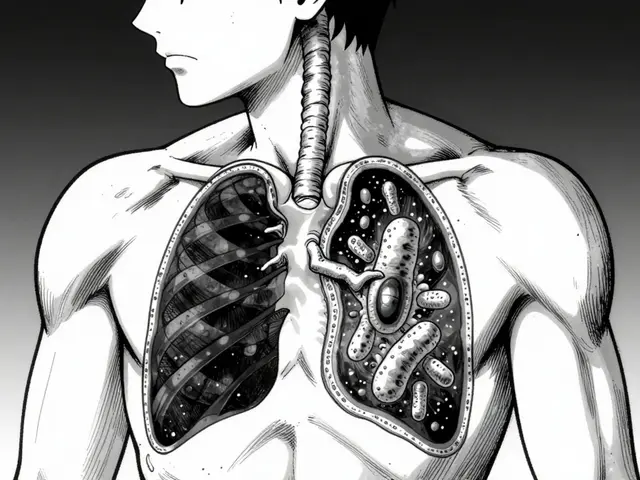
Rifampin Drug Interaction Simulator
How it works: Rifampin triggers the production of CYP3A4 enzymes in the liver. This "super-charges" your metabolism, clearing other medications out of your blood faster. Select a medication below to see the estimated impact on its effectiveness.
Select Medication
Interaction Analysis
Please select a medication from the list to visualize the impact of Rifampin.
🔬Select a drug to see details.
Note: This is a simulation based on average clinical data. Actual interactions vary by individual and dosage.
Imagine taking a life-saving medication for tuberculosis, only to find that it quietly cancels out your birth control, thins your blood less effectively, or makes your HIV medication stop working. This isn't a rare fluke; it's a known biological side effect of Rifampin is a powerful semi-synthetic antibiotic used as a cornerstone for treating drug-sensitive tuberculosis. Also known as Rifampicin, it fundamentally changed TB care by slashing treatment times from 18 months down to just six. However, while it's an expert at killing bacteria, it's equally expert at changing how your liver processes other drugs.
The Engine Behind the Interaction: Enzyme Induction
The primary reason rifampin causes so many problems with other meds is a process called enzyme induction. To understand this, think of your liver as a processing plant with various "machines" (enzymes) that break down medications. Rifampin doesn't just use these machines; it tells your body to build hundreds of new ones.
This happens because rifampin activates a specific sensor in your cells called the Pregnane X Receptor (or PXR), which is a nuclear receptor that regulates drug metabolism. When PXR is triggered, it ramps up the production of CYP3A4, the most important cytochrome P450 enzyme responsible for metabolizing a huge variety of pharmaceutical drugs. Within just 72 hours of your first 600 mg dose, your CYP3A4 activity can jump by 200% to 400%.
Because your liver is now "super-charged," it clears other medications out of your system much faster than normal. If a drug is metabolized by CYP3A4, rifampin essentially acts like a vacuum, sucking that medication out of your bloodstream before it ever has a chance to work.
Which Medications Are Most at Risk?
Not every drug is affected, but those that rely on the CYP3A4 pathway are in trouble. The drop in plasma concentrations can be staggering. For instance, the effectiveness of oral contraceptives can plummet by about 67%, leading to unplanned pregnancies. Similarly, the blood-thinning effects of Warfarin, an anticoagulant medication used to prevent blood clots, can be reduced by 42%.
The most critical interactions often occur with HIV protease inhibitors, where drug levels can drop by 75% to 90%. In a clinical setting, this can lead to treatment failure and the development of drug-resistant viral strains. This is why doctors must meticulously review every single pill, supplement, or hormone therapy a patient is taking before starting a TB regimen.
| Medication Type | Estimated Reduction in Plasma Levels | Clinical Risk |
|---|---|---|
| Oral Contraceptives | ~67% | Unintended Pregnancy |
| Warfarin (Blood Thinners) | ~42% | Increased Clotting Risk |
| HIV Protease Inhibitors | 75% - 90% | Treatment Failure / Resistance |
The Paradox of Bacterial Tolerance
While rifampin is fighting the disease, the bacteria themselves fight back in a way that complicates treatment. Mycobacterium tuberculosis, the bacterium that causes tuberculosis, can develop a level of tolerance to the drug very quickly. Within just 48 hours of infecting macrophages, the bacteria start using "efflux pumps"-essentially microscopic sump pumps-to kick the rifampin right back out of the cell.
Even stranger, rifampin can actually cause some bacteria to become more tolerant of it. By triggering the upregulation of the rpoB gene, the drug creates a subpopulation of "survivors." This is a paradoxical effect: the very drug used to kill the bacteria is helping some of them survive. This is why a strict six-month regimen is non-negotiable; cutting treatment short can lead to relapse rates higher than 25%.
Liver Health and Unexpected Benefits
Adding a potent enzyme inducer to your system isn't always easy on the liver. About 10% to 20% of patients see a significant spike in liver enzymes (ALT >3x the upper limit of normal), signaling potential drug-induced liver injury. This happens due to oxidative stress and mitochondrial dysfunction caused by the drug's metabolic demands.
Interestingly, this "side effect" of enzyme induction is sometimes used as a tool. In patients with cholestatic liver diseases, rifampin is occasionally used off-label to treat severe itching (pruritus). By inducing CYP3A, it helps the liver hydroxylate bile acids more efficiently, reducing their reabsorption in the gut by about 40% and providing relief for up to 80% of patients with primary biliary cirrhosis.
Managing the "Washout" Period
One of the biggest mistakes patients or providers make is assuming that once the rifampin stops, the interactions stop too. The enzymes rifampin creates don't just vanish the moment you swallow your last pill. Because these induced proteins have a relatively long half-life, the "super-charged" state of your liver persists for a while.
Generally, you need a washout period of about two weeks before introducing sensitive medications. For drugs with a narrow therapeutic index-where the difference between a working dose and a toxic dose is tiny-a four-week window is often recommended. Starting a new, sensitive medication too early can lead to unpredictable blood levels as the liver slowly returns to its baseline metabolic rate.
New Frontiers: Breaking the Tolerance
Researchers are currently looking for ways to stop the bacteria from pumping rifampin out of their cells. Recent studies have looked into using Verapamil, a calcium channel blocker typically used for high blood pressure, as an adjunctive therapy. In lab settings, verapamil has shown it can block those bacterial efflux pumps.
Even more promising are Proton Pump Inhibitors (PPIs), like Omeprazole, a medication used to reduce stomach acid. Omeprazole has been shown to inhibit rifampicin efflux by about 68%. If these findings translate from murine models to humans, we might be able to shorten the grueling six-month TB treatment by 50% while keeping relapse rates extremely low.
Should I take rifampin with food?
It is best to take rifampin on an empty stomach. Taking it with food can reduce the amount of drug your body absorbs by about 30%, which might make the treatment less effective against the bacteria.
How long does it take for rifampin to start affecting other drugs?
The induction process begins quickly. Changes in mRNA levels in your blood cells can be seen within 24 hours, and a significant increase in enzyme activity usually occurs within 72 hours.
Does rifampin cause permanent liver damage?
While rifampin can cause drug-induced liver injury (DILI) and elevated liver enzymes in 10-20% of patients, this is typically monitored through regular blood tests. In most cases, the injury is reversible once the medication is stopped or adjusted.
Can I use a backup contraceptive while on rifampin?
Yes, and it is highly recommended. Because rifampin reduces the effectiveness of oral contraceptives by roughly 67%, using a non-hormonal barrier method (like condoms) is essential to prevent unplanned pregnancy.
Why can't I just take rifampin for 3 months instead of 6?
Shortening the treatment too much is dangerous because of "antibiotic tolerance." The bacteria can hide or pump the drug out of their cells; cutting treatment below 4 months has been shown to increase relapse rates to over 25%.